| Translation-driven insights across the cell and gene therapy lifecycle Cell & Gene Therapy Insights is an online, open-access, peer-reviewed journal dedicated to the interdisciplinary exploration and advancement of cell and gene therapy. Through translational focus, we bridge academia and industry to support preclinical and clinical development, scale-up, and commercialization. Register below to access all of our content for free. Contact us |  |
May 2026
Upcoming webinars

High-throughput affinity chromatography screening: boosting AAV vector recovery from 70%
Alésia Xemaire, Nicolas Laroudie
10 June
in 2
Days
Turning biological variability into consistent outcomes with cell culture vessels
Paulina Zatarain
11 June
in 3
Days

Human serum albumin: a trusted biomaterial for cell therapy and beyond
Alejandra Gutierrez-Guerrero, PhD
16 June
in 8
Days

From bench to 1,000 L: maintaining CQAs and controlling COGS in AAV and LVV scale
E Ayuso, DVM, PhD, N DePrimo, MSc, M Brunati, PhD et al.
17 June
in 9
Days
Optimizing CRISPR/Cas9 cell line development with microfluidic single-cell sorting
Courtney J. Haycraft, PhD, Bhamini Purandare, MSc
18 June
in 10
Days

Accelerating AAV biosafety and characterization decisions with validated NGS workflows
Andrew Hillhouse
30 June
in 22
Days
Latest Articles

Rapid sterility & mycoplasma testing in cell therapy
4 June

Building CAR‑T therapies with GMP‑first thinking
Stefanos Theoharis
3 June

Towards intelligent supply networks: AI‑enabled simulation in the evolution of digital twins for autologous cell therapy manufacturing
K Wang, Z Li, C White et al.
1 June

Event Preview – Cell & Gene Therapy World Asia
1 June

Industrialization of cell therapy manufacturing: from artisanal process to scalable medicine
Sapna Tandon
28 May

In vivo CAR-T: toward scalable and programmable immunotherapy
Kartika Venugopal
26 May
Bending the cost curve in AAV manufacturing via scalable platform innovation, productivity gains, and analytical insight
Vijetha Bhat
26 May

From bottleneck to breakthrough: how downstream process innovation, analytics, and AI are reshaping AAV‑based gene therapy
S Jeffers, S Mohanty, J Senaratne et al.
21 May
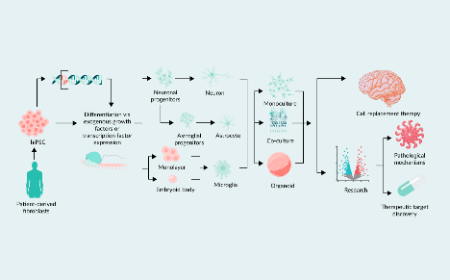
Human iPSC models of neurodegenerative disease: from application to therapy
D M Alliband, L J Willoughby, J D Lane et al.
21 May
Latest channel content
| Your life sciences content marketing partner We go beyond providing the informative content in our journals. We can help you engage your audience through tailored webinars and roundtables that generate qualified leads, showcase your company's expertise, and spark meaningful discussion on key scientific and regulatory topics. Ready to amplify your brand's impact? View our media kit |  |
| Our journals Our portfolio of four open access journals provides trusted insight across the advanced therapies landscape. Cell & Gene Therapy Insights, Bioconjugate Insights, Vaccine Insights, and Nucleic Acids Insights deliver expert commentary, original research, and practical guidance that help researchers, developers, and manufacturers stay aligned with the rapidly evolving needs of modern biomedicine. Each journal focuses on translating innovation into real-world impact, giving readers clear, actionable knowledge that supports progress from discovery through to clinical and commercial success. |  View View |  View View |  View View |  View View |
FAQ |
| Stay informed Want to keep up with the latest news in biopharma? Register for free to get the latest news, views and updates from your field. |
| Bioconjugate Insights | Cell & Gene Therapy Insights | Nucleic Acid Insights | Vaccine Insights |