Cell & Gene Therapy Insights is an online, open-access, peer-reviewed journal dedicated to the interdisciplinary exploration and advancement of cell and gene therapy. With a translational focus, we connect innovative research to practical clinical applications, providing valuable insights into one of biotechnology’s fastest-evolving fields.
We address the key challenges and latest developments across advanced therapies, publishing original research articles, expert reviews, commentary, clinical trial reports, and more. Visit the Cell & Gene Therapy Insights Journal page for our complete collection.
Our popular webinar series provides expert-led discussions on important developments and methodologies in the field, designed to support ongoing professional growth.
Explore our specialised channels, including detailed coverage of critical areas like the cell and gene supply chain, for targeted insights into manufacturing, logistics, and regulatory frameworks essential to therapy commercialisation.
Learn more about our journal’s mission and publishing criteria by visiting our aims and scope.
Sign-up for free to gain unlimited access to our extensive library of articles, webinars, podcasts, news, and interviews, and stay at the forefront of cell and gene therapy innovation.
If you’re interested in working with us, from sponsoring articles to webinars and more, view the media kit to find out more.
March 2026
Upcoming webinars

Data-driven platform selection for automated cell therapy manufacturing
Strengthening ATMP process development through real-time metabolic monitoring and control

Data-driven platform selection for automated cell therapy manufacturing (APAC)

Have we finally reached the end of in vitro testing? Positioning NGS in cell and gene therapy biosafety testing

Improving manufacturing reliability in cell and gene therapy: practical operational strategies

Novel resin design enables efficient enrichment of full AAV capsids by anion exchange chromatography
Latest Articles

Industry Insights: Regulatory dynamics and clinical progress in early 2026

Tailored analytical strategies for AAV aggregation: purpose‑driven method selection for enhanced product development
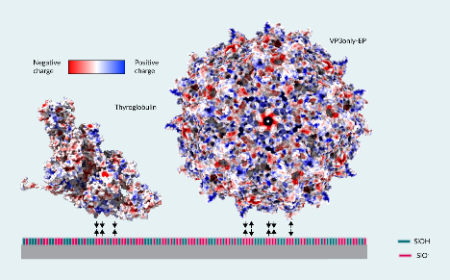
New analytical method for rAAV titer and empty/full ratio determination in cell lysate and conditioned medium

Advancing AAV manufacturing through platform design and process understanding

Engineering confidence in the next era of AAV-based gene therapy

Choosing a biomanufacturing service organization: from the BSO perspective

Building confidence in cell and gene therapy: USP’s role in an evolving therapeutic frontier

Editor’s picks: exploring in vivo cell and gene therapies